| Q: |
What is a miscarriage?
| | A: |
A miscarriage is the spontaneous loss of a baby at any time up
until the 24th week of pregnancy. After 24 weeks the loss is referred to
as a stillbirth. The signs of a miscarriage are vaginal bleeding and
periodlike cramps. As not all miscarriages follow the same pattern,
there are various terms to describe what occurs:
A threatened miscarriage occurs when there is bleeding and possibly pain, but the fetus survives.
An inevitable miscarriage occurs when there is bleeding and pain due to contractions in the uterus, the cervix opens, and the fetus is expelled.
A missed miscarriage occurs when the fetus dies but remains in the womb and either is expelled naturally later or removed by surgery.
|
| Q: |
I've recently miscarried—why did this happen?
| | A: |
Miscarriage occurs in 10–20 percent of pregnancies. In the vast
majority of these the cause is never identified, but it's unlikely to be
related to anything you did or didn't do. There are thought to be
several reasons why miscarriages occur.
There may be a genetic problem, in which the baby or placenta doesn't
develop normally; levels of the pregnancy hormone progesterone may be
low; there may be an immune disorder in which the mother's immune system
reacts against the pregnancy; an infection may be present; or there may
be problems with the uterus or cervix. Miscarriages tend to be more
common in older women.
Share Pregnancy and Infant Loss Support (www.nationalshareoffice.com)
offers support, advice, and information about miscarriage. You may feel
comforted to know that, statistically, any future pregnancy you have is
likely to progress normally.
|
| Q: |
My period was late and now I'm bleeding really heavily—could I be having a miscarriage?
| | A: |
In the absence of a positive pregnancy test or a pregnancy
confirmed by an ultrasound scan, it is difficult to know whether or not
you were pregnant. If you have had unprotected intercourse in the time
since your last period, it is possible that you could have been pregnant
and this is a miscarriage. The lateness of your period may be a clue,
but won't confirm one way or another. If you have any other symptoms of
pregnancy it might be worth doing a pregnancy test since sometimes, even
when there has been bleeding, a viable pregnancy is discovered.
However, it could also be a
late period for no other reason than that this happens on occasion to
everyone. A delayed period can be caused by weight loss or gain, stress,
or if you have been taking an oral contraceptive pill but missed a
dose.
Talk to your midwife
or doctor if the bleeding continues; you feel faint or experience
palpitations; your period lasts for longer than seven days; you have
more than six well-soaked pads a day; or if you have any severe
abdominal pain. Your doctor can do a blood test to check your iron
levels and possibly determine if you have been pregnant, in which case
an incomplete miscarriage ectopic pregnancy will need to be ruled out
.
|
| Q: |
I'm 10 weeks pregnant and getting cramping pains. Do I need to rest to avoid a miscarriage?
| | A: |
Cramping pains on their own without vaginal bleeding or spotting
can occur at this stage of pregnancy. Sometimes pain can be felt as the
ligaments stretch when the baby and your uterus grows. There are also
other possible causes for the pain aside from miscarriage, such as
constipation or a urinary tract infection.
Many doctors advise rest to
avoid a “threatened” miscarriage, but there is no strong evidence that
this will make any difference to the outcome of a pregnancy. If you feel
like resting because you are in discomfort from the cramping pains then
do rest, but if you feel happy to continue as you normally would then
that may be the best option for you. Soaking in a warm bath and
practicing relaxation techniques may ease the intensity of the pain. If
the pain increases or you get any bleeding or spotting, contact your
doctor.
|
| Q: |
Does bleeding in pregnancy mean that miscarriage is inevitable?
| | A: |
No, many women experience bleeding in early pregnancy and then
proceed to have a healthy pregnancy and baby. Indeed, some women have
intermittent bleeding throughout pregnancy.
Despite this, any
bleeding should be investigated. This is usually done with an ultrasound
to determine if the pregnancy is viable and to identify if there is any
indication of where the bleeding is coming from. In very early
pregnancy, it can be hard to see the pregnancy on an ultrasound and a
blood test to measure levels of the pregnancy hormone human chorionic
gonadotrophin (HCG) may be done, mainly to rule out the possibility of
an ectopic pregnancy.
Unfortunately for you, this is a time of waiting; the timing of any
further scans is usually determined by the findings of the initial scan
and the blood tests and the symptoms you are experiencing.
|
| Q: |
I've had three miscarriages before and I'm scared of trying again—is there anything I can do?
| | A: |
It is understandable given your experiences that trying to get
pregnant again is a scary proposition. Following a third miscarriage, it
is usual for your doctor to offer you a number of investigative tests
to see if a reason for the miscarriages can be found. In some cases, a
cause is identified and treatment can be offered to help improve the
outcome for subsequent pregnancies.
You are likely to be
given a number of blood tests. These are to look for antibodies
(proteins in the blood that fight any substance they recognize as
foreign to your body), chromosomal abnormalities, and infection. You may
also have a vaginal examination and swab and an ultrasound scan to
check your womb and tubes. If a chromosomal abnormality is found,
genetic counseling should be offered to discuss the implications for
future pregnancies. The levels of the hormones progesterone and
prolactin may also be checked since these can play a role in
miscarriage. Sometimes, the cervix is found to be weakened and likely to
open early. If this is the case, you may be offered a cervical stitch
that acts like a drawstring on the cervix and hopefully prevents future
miscarriage or premature delivery.
If you haven't
already been offered these tests, talk to your doctor about them before
trying to get pregnant again so that you can begin any recommended
treatment as soon as possible.
|
| Q: |
My mom had two miscarriages—does that mean I am more likely to miscarry?
| | A: |
Ask your mom if she was given any particular reason for her
miscarriages. If, for example, she knows that they were due to a
chromosomal abnormality, such as sickle-cell disease, or if she had a
medical condition, such as heart disease, then there is a possibility
that the condition is hereditary and the risk of miscarriage may be the
same for you too.
However, it's most
likely that your mother's miscarriages were unfortunate chance
occurrences for which no reason was found. If this is the case, then you
are at no more risk of experiencing a miscarriage than any other woman
your age. However, if you do become pregnant, it would be worth
mentioning your mother's pregnancy history at your initial prenatal
appointment, since your family medical history is an important part of
your medical record during pregnancy.
|
| Q: |
I've had several miscarriages and my doctor has referred me to a genetic counselor—why?
| | A: |
A genetic counselor is a highly trained professional who supports
families before and after conception. Often a miscarriage is caused by a
genetic abnormality in the fertilized egg or embryo. This is usually a
one-time occurrence and can affect anyone. However, if a woman has
recurrent miscarriages, it may be that she is carrying a genetic
condition.
Women and their
partners are referred to a genetic counselor if either partner has a
condition that can affect future children or the chances of becoming
pregnant or continuing with a pregnancy since they may be more likely to
miscarry or be offered a termination. For example, if there is a
history of sickle-cell disease, a blood disorder that causes chronic
anemia and increases the risk of a preterm birth and health problems in
the baby, it may be that either or both parents are carrying a gene that
can affect a baby.
A genetic counselor
helps you understand how your genes could affect conception and
pregnancy and about the tests available to determine if a fetus is
affected. The counselor will discuss a range of issues, including the
moral and ethical issues related to genetic testing, since it is common
for couples to feel stress, guilt, and confusion in this type of
situation.
|
| Q: |
I lost my baby, but I want to get on and try again—is this OK?
| | A: |
Although there are no hard rules about when to try for another
baby, it is important that you allow yourself time to grieve and your
body to recover before trying to conceive again. Some women feel able to
try again within a month, while others may not feel ready for at least a
year. Whatever you feel, it's wise to let your hormones and body settle
down after a miscarriage before considering another pregnancy. The
usual advice is to wait for at least three months before trying to
conceive again so that you feel both emotionally and physically prepared
for another pregnancy. Your partner also needs to feel that the time is
right for you both to try again.
|
| Q: |
We had a miscarriage at 20 weeks. Will the doctors find the cause so that we can move on?
| | A: |
Coping with the loss of a baby well into pregnancy is difficult
and upsetting. Many women ask themselves why a miscarriage happened and
feel unable to move on until that important question is answered.
Unfortunately, unless this was a recurrent miscarriage of three or more,
there may not be an investigation, although it may be suggested that
you have a cervical stitch in future pregnancies to stop the cervix from dilating too early
.
It may be worth
talking to a counselor who is trained to support women and families
through such difficult times; your doctor or midwife may be able to
refer you. You may find that discussing your miscarriage directly with a
health professional helps to answer any concerns you or your partner
have, and by communicating in this way you will have started to move
forward and may begin to feel able to consider planning another
pregnancy.
|
| Q: |
My partner had a miscarriage. I'm being supportive but I'm devastated too. What should I do?
| | A: |
Dealing with a miscarriage is very difficult for both women and
men, but often far more attention is given to a woman, and a man's
feelings are simply ignored. However, it's important that you don't
internalize your loss and do acknowledge your feelings, which may range
from feeling scared, disappointed, and out of control, to blaming
yourself for not being supportive enough and mourning your loss of
identity as a father. Although you want to support your partner, you
also need to recognize your own need to grieve, as working through your
emotions can help you to come to terms with your loss more quickly.
A good support network is
also important for both of you and it can help to find a sympathetic
listener outside of your relationship. Initially, you may find
discussing your feelings with another male easier than talking to your
partner. You could also talk to your doctor or to a trained counselor
for additional support.
|
| Q: |
What is a “D and C”?
| | A: |
D and C stands for dilation and curettage, a surgical procedure
in which the opening to the uterus, called the cervix, is stretched
(dilatation) and the tissue that lines the uterus is scraped or removed
(curettage). This procedure is sometimes carried out after a miscarriage
to ensure that any of the remaining products of the conception and
pregnancy have been removed.
There are
advantages and disadvantages to consider before having a D and C. The
procedure is usually completed within two hours and most women resume
their usual activities within a week. However, the need for routine
surgical evacuation, or a D and C, following a miscarriage has been
questioned because of potential complications, such as bleeding and
infection. Ask your doctor for advice. There are less invasive options
than a D and C for dealing with a miscarriage. One method is simply to
watch and wait to see if the uterus will spontaneously expel any
remaining products of conception. Another option is a drug treatment
that works by stimulating the uterus to contract and naturally expel
pregnancy tissues.
|
The risk of miscarriage What can increase the likelihood of a miscarriage?
There are several factors that can increase your risk of miscarriage.
Older women have an
increased risk of having a miscarriage. It is thought that this is
largely due to the fact that older women are more likely to have babies
with chromosomal abnormalities, which may have problems developing and
miscarry. Some underlying medical conditions can also increase your
chances of miscarriage, such as polycystic ovary syndrome or fibroids.
Other factors that can increase your risk are if you are particularly
underweight or overweight, smoke, drink heavily, or take recreational
drugs. Miscarriages are also more likely the more pregnancies you have
had.
Talking to others Coming to terms with your loss
Losing a
baby during pregnancy can be devastating, leading to feelings of grief
such as anger, depression, guilt, and anxiety. Talking to others can
help you to work through your feelings.
Ask your midwife or doctor to put you in touch with a counselor who specializes in pregnancy loss. Let close friends and family members know how you are feeling.
Share Pregnancy and Infant Loss Support is a great source of support. Talk to your doctor or midwife about why the miscarriage may have happened.
NOTE
One in four women miscarry in their first pregnancy. In most cases, women go on to have successful pregnancies
NOTE
Talking about your experience of miscarriage rather than keeping it to yourself can help the healing process
Possible causes of miscarriage Losing a baby in pregnancy
About 1 in 4 first
pregnancies ends in miscarriage, generally within the first 12 weeks.
Often no cause is identified and may not be investigated unless a woman
has had three or more miscarriages in a row, known as “recurrent
miscarriages”.
| Q: |
Why has it happened?
| | A: |
Some miscarriages occur because of a one-time genetic problem
(caused by a faulty chromosome) when the baby does not develop properly.
Genetic problems account for 60 percent of early miscarriages. If you
think this may have been the cause, you can request tissue tests from
the baby. Based on these results, you may be able to receive specialized
counseling to discuss the risk of it happening again (see Genetic Counselor).
After 12 weeks, the chances of you losing your baby because of a
chromosomal disorder reduce to about 10 percent; however, if you are
over 35, this risk is higher. Other less common causes of miscarriage
include fibroids (noncancerous growths), infection, problems with the
uterus, hormonal imbalances, and immune system disorders. An ectopic pregnancy occurs when the embryo implants in a fallopian tube and needs to be removed.
|
| Q: |
What can cause late pregnancy loss?
| | A: |
A late pregnancy loss (referred to as a stillbirth after 24
weeks) can be due to the cervix being weak (or “incompetent”), causing
the cervix to dilate too early. This accounts for 15 percent of repeated
miscarriages. In future pregnancies, a stitch around the cervix can
strengthen this muscle and prevent it from opening early. Another cause
of a late miscarriage can be if the placenta does not function properly
and affects the baby's growth.
|
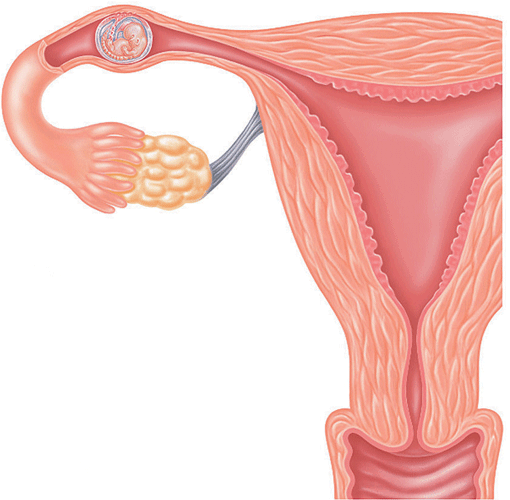
Ectopic pregnancy
Implanting outside of the uterus
In 99 percent of ectopics, the egg implants in a fallopian tube, see the
image;
rarely it implants in the cervix or an ovary. An ectopic pregnancy can
rupture a tube, and needs swift medical attention to remove it.
|