You are 8 Weeks and 2 Days 222 days to go…
Who will your baby look like? His unique facial features are beginning to take shape this week.
Your baby today
The baby’s hands (seen here) and feet are gradually developing and they are formed of cartilage, not bone at this early stage. In the center left, the fused rays of the hand plate that will become the fingers can be seen. The ribs are in the background.
If you were to have an ultrasound scan this week, it would be possible to recognize several of your baby’s facial features.
His eyelids fuse and will remain closed until around the 26th week. The lips have already formed and with the surrounding skin will have the greatest concentration of nerves. The muscular tongue arises from the base of your baby’s mouth, but it will be two weeks before the first taste buds appear. The hard palate that forms the roof of the mouth arises from two “shelves” that start to grow, one each side, beneath the tongue; these shelves will lift upward to connect horizontally, allowing the tongue to drop down in to the mouth. Once they have joined together, the septum of the nose grows downward to meet them.
Your baby’s tiny tooth buds are in place and this is critical to adequate jaw development. One branch of tooth buds will form the first milk teeth and a separate branch will eventually form the permanent teeth. The milk teeth develop slowly and it will not be until the six month of pregnancy that they acquire their hard enamel coating.
The embryo is still very curled up, with the head resting on the chest. Over the next two weeks as the jaw and neck grow, the head will gradually lift.
… Doctor
| Q: | I work for a dry cleaner. Could the chemicals harm my unborn baby? |
| A: | Concerns about dry-cleaning chemicals stem from research showing that women who operated dry-cleaning machines had a higher risk of miscarriage. If touched or inhaled, some organic (carbon-containing) solvents used in dry-cleaning machines can pass through the placenta and some are thought to increase the risk of miscarriage or birth defects. Talk to your employer to find out how your duties can be changed for the duration of your pregnancy to limit your contact with organic solvents and industrial chemicals. |
Childhood illnesses
Having immunity against common infectious illnesses will protect your unborn baby. You may have natural immunity from having conditions such as chicken pox and fifth disease as a child. You will almost certainly have been vaccinated against mumps and measles, so your unborn baby will be protected from these.
If you are unsure about your immunity or medical history, or think you may have been in contact with any of these infections, contact your doctor immediately for further advice. He or she will be able to do a checkup and provide reassurance.
If you are in regular contact with young children while you’re pregnant, it’s even more important that you check your immunity to childhood illnesses.

You are 8 Weeks and 3 Days 221 days to go…
It’s a few weeks before the hormone responsible for morning sickness subsides, but the nausea will pass soon.
Your baby today
In a matter of days, your baby’s eyes have developed from slight ridges to clear depressions, on each side of the face. The face is developing rapidly at this stage, and your baby’s heartbeat would be seen on an ultrasound scan.
You may be wondering when you’ll wake up and no longer feel sick. HCG (human chorionic gonadotrophin) levels, which may be responsible for feelings of nausea will begin to fall in about three weeks’ time and most women begin to feel better then. For some women the sickness may continue beyond this time.
You may have just started to feel nauseous or your sickness may have begun weeks ago and now be worse, but by around week 12 you should be over the worst. Nausea that happens daily, especially if it is associated with fatigue, can be very wearing so try to remember that it’s temporary. It’s normal to have some morning sickness and you should be able to keep some foods and fluids down. However, for a small minority of pregnant women—about 1 percent—the vomiting is severe, occurring regularly and lasting over a period of weeks. This more serious form of morning sickness is called hyperemesis gravidarum and can lead to dehydration. Hospital treatment with intravenous fluids and anti-nausea drugs may be required to rehydrate you.
Seek advice from your doctor if you’re concerned about the amount of times you’re vomiting or if you’re struggling to keep fluids and food down.
Acupressure wristbands
A simple solution to help relieve feelings of nausea is to wear acupressure wristbands. Available from pharmacists, these bands have been clinically tested in the treatment of pregnancy-induced nausea. Unlike anti-nausea drugs, they don’t have any side effects and are easy to use.
The elastic bands, one worn on each arm, work by applying pressure on the Nei Kuan acupressure point (known as P6). They can be washed and reused as necessary.

… Health
Fit—not sick
If you’re feeling particularly nauseous, try going for a brisk walk in the fresh air while concentrating on your breathing and posture. Sometimes frequent sips of water help these feelings, and will allow you to exercise longer. Regular exercisers may find that nausea is absent during exercise, although it may resume after the session.
Extreme nausea and vomiting can be a sign of overexercising. Always drink water before, during, and after any physical activity.
About 70–80 percent of pregnant women suffer from morning sickness.
If you are one of the 20–30 percent who don’t be thankful. You may get anxious if you’re not feeling sick because it is such a common symptom, but don’t worry and just count yourself lucky.
Your Baby’s Life Support System
The placenta links your baby’s blood supply to your own and carries out all the functions that your baby can’t perform for himself. The placenta is rooted to the lining of your uterus and linked to the baby by the umbilical cord.
How the placenta develops
The placenta forms from cells in the embryo shortly after the egg implants in the lining of the uterus. Early placental growth is rapid, and at the beginning of the first trimester, the placenta is larger than the baby. However, the baby’s growth catches up by 16 weeks, and by the end of pregnancy the baby is almost six times heavier. The final weight of the placenta is between 12 oz (350 g) and 1 lb 5 oz (600 g). Once its structure is complete at the end of the first trimester, it takes on many important functions for the rest of the pregnancy.
Growth after the first trimester
The placenta grows throughout the second trimester. By the third trimester, growth slows, but placental efficiency continually improves as extra villi grow and increase the available surface area of the placenta by nearly fourfold. Cell layers also become thinner so that substances can be exchanged efficiently.
Placental blood flow is massive and many of the changes in your circulation are designed to meet its needs. By term, a tenfold increase in placental blood supply results in a fifth of your circulation supplying the placenta with up to half a liter of blood (almost a pint) each minute.
The aging placenta
The placenta ages towards the end of pregnancy, especially after 40 weeks. However, at least 60–80 percent of its function would need to be lost before there were any signs of problems with blood flow in the umbilical cord.
The role of the placenta
The placenta fulfills many essential roles that help sustain your pregnancy and enable your baby to grow and develop.
The exchange of substances
The placenta transports substances to and from your baby, acting as your baby’s lungs, kidneys, and digestive system.
To obtain oxygen, the baby’s blood cells grab oxygen molecules from your own hemoglobin (the oxygen-carrying substance in blood). Fetal hemoglobin has a modified structure that makes it bind readily to oxygen. Your baby requires twice as much oxygen weight for weight as your own needs so the transfer of oxygen needs to be efficient. The placenta’s enhanced blood supply, large surface area, and the characteristics of fetal hemoglobin all ensure the efficient transfer of oxygen from mother to baby.
As your hemoglobin gives up oxygen, it accepts carbon dioxide molecules. Your lungs breathe out air rich with the baby’s carbon dioxide as well as your own and the cycle begins again.
To grow and develop your baby also needs amino acids, the building blocks for proteins, and minerals like calcium and iron and these all pass from your own circulation via the placenta to the baby.
Protecting your baby
The placenta protects your baby from infections and harmful substances. Since your baby hasn’t encountered any external threats he doesn’t yet make protective antibodies known as immunoglobulins that can identify threats, such as viruses or bacteria. Instead he is reliant on the transfer of immunoglobulins from your circulation via the placenta and into his circulation. This means that you are able to protect your baby in the uterus from illnesses such as chickenpox. After your baby is born, the immunoglobulins he acquired from you will eventually be lost, which means that later as a child he becomes susceptible to chickenpox.
Hormone production
The placenta produces hormones, such as estrogen and progesterone, that are vital to your baby’s well-being and lead to many of the changes in your body during pregnancy.
Heat transfer
A baby’s high metabolic rate generates heat. The placenta’s big surface area and high blood flow disperses heat, controlling the baby’s temperature.
How substances are exchanged in the placenta
Inside the placenta
The placenta contains a huge network of tiny projections called chorionic villi that branch out from a thin membrane, the chorion, and contain fetal blood vessels. The chorionic villi are bathed in maternal blood within the intervillous space. Each villus is only one or two cells thick, which allows the transfer of gases and nutrients between the mother and the baby, while ensuring that the two circulations never come into direct contact. Through the process of diffusion, oxygen and nutrients such as glucose, your baby’s primary source of energy, from the mother pass into the fetal circulation, and waste products from the baby are picked up and carried away in the mother’s bloodstream. The chorionic membrane also acts as a protective barrier, preventing many harmful substances and infections from reaching the baby.
The vast network of villi in the placenta facilitates the transfer of gases, nutrients, and waste products to and from your baby.
Structure and function
The umbilical cord
The umbilical cord, which connects your baby to the placenta, contains three vessels: two arteries, which carry blood from the baby to the placenta, and one vein, which carries blood back to the baby. The blood in the arteries contains waste products, such as carbon dioxide, from the baby’s metabolism. Carbon dioxide is transferred across the placenta to your bloodstream and then to your lungs, where it’s breathed out. Oxygen is transported from red bloods cells in your circulation, across the placenta to the baby in the umbilical vein. In addition to oxygen, the umbilical vein transports nutrients from the placenta to your baby.
The vessels in the umbilical cord have a protective coating called Wharton’s jelly, and the cord is coiled like a spring so that the baby is free to move around. The coiling pattern of the cord has usually established itself by week nine and is usually in a counterclockwise direction. However, the cord can coil later, and sometimes isn’t established until 20 weeks. The baby’s movements seem to encourage the cord to coil.
The cord is usually attached to the center of the placenta, although sometimes it’s attached near the edge. Very occasionally, it divides into its separate vessels before finally entering the placenta. The cord is usually under 1 in (1–2 cm) in diameter and 23 in (60 cm) long, which is twice the length needed to ensure that there are no problems at delivery.
After delivery, the cord vessels close by themselves. The arteries close first, helped by their thicker muscular walls. This prevents blood loss to the placenta from your baby. The umbilical vein closes slightly later (starting at 15 seconds, but only completed by 3 or 4 minutes). This allows blood to continue to return to your baby during the first few minutes of life. As a result, many feel that a slight delay before clamping the cord can be beneficial to the baby. There are no nerves within the cord, so cutting the cord after delivery is a painless procedure for your baby.
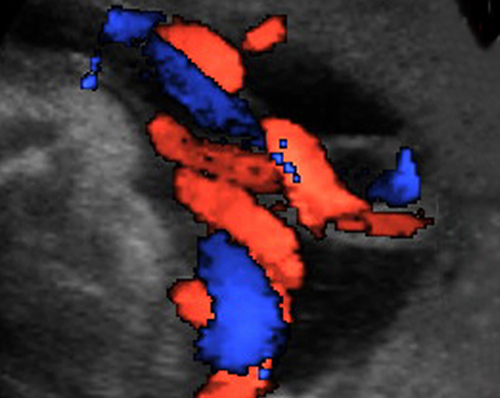
This Doppler scan shows the blood vessels in the umbilical cord. Blood flows through a single vein (blue) and two arteries (red).
Some harmful substances can cross the placenta
For this reason, it’s important that you protect your baby by taking medical advice before you use any type of medication during pregnancy.