How Pregnancy Affects Your Sexual Desire
Pregnancy and sex. Has your sexual
desire increased? Is sex the last thing on your mind? Generally, women
experience one of two sex-drive patterns during pregnancy. One is a
lessening of desire in the first and third
trimesters, with an increase in the second trimester. The second is a
gradual decrease in desire for sex as pregnancy progresses.
During the first trimester, you may
experience fatigue and nausea. In the third trimester, your weight
gain, enlarging abdomen, tender breasts and other problems may make you
desire sex less. This is normal. Tell your partner how you feel, and
try to work out a solution that pleases you both. Tenderness and
understanding can help.
Pregnancy enhances the sex drive for some
women. A woman may experience orgasms or multiple orgasms for the first
time during pregnancy. This is due to heightened hormonal activity and
increased blood flow to the pelvic area.
When to Avoid Sexual Activity
Some situations should alert you to
refrain from sexual activity. If you have a history of early labor,
your healthcare provider may warn against intercourse and orgasm;
orgasm causes mild uterine contractions. Chemicals in semen may also
stimulate contractions, so it may not be advisable for a woman’s
partner to ejaculate inside her.
If you have a history of miscarriage,
your healthcare provider may caution you against sex and orgasm.
However, no data actually links sex and miscarriage. Your healthcare
provider may advise no sex if you have certain pregnancy problems.
Some sexual practices should be avoided
when you’re pregnant. Don’t insert any object into the vagina that
could cause injury or infection. Blowing air into the vagina is
dangerous because it can force a potentially fatal air bubble into a
woman’s bloodstream. (This can occur whether or not you are pregnant.)
Nipple stimulation releases oxytocin, which causes uterine
contractions; discuss this practice with your healthcare provider.
An Incompetent Cervix
An incompetent cervix refers to painless
premature dilatation (stretching) of the cervix, which usually results
in delivery of a premature baby. Usually the problem doesn’t happen
until after the 16th week of pregnancy. The woman doesn’t
realize the cervix has dilated until the baby is delivering; it often
occurs without warning. Diagnosis is usually made after
one or more deliveries of a premature infant without any pain before
delivery. Fortunately, an incompetent cervix is relatively rare.
If this is your first pregnancy, there’s
no way to know whether you have the problem. The cause of cervical
incompetence is usually unknown. Some experts believe it occurs because
of previous injury or surgery to the cervix, such as dilatation and
curettage (D&C) for an abortion or a miscarriage. If you’ve had
problems in the past or have had premature deliveries and have been
told you might have an incompetent cervix, share this important
information with your healthcare provider.
Ultrasound may be used to measure the
cervix. If a woman’s cervix is shorter than normal, the condition is
sometimes described as a short cervix or shortened cervix.
Treatment for an incompetent cervix is usually surgical. The weak cervix is closed with a McDonald cerclage.
A suture, similar to a “pursestring,” is stitched around the cervix to
keep it closed. The procedure is usually performed in a hospital
operating room or in labor and delivery. General anesthesia or I.V.
sedation is given. The procedure takes about 30 minutes; after it’s
over, you’ll probably be monitored for a few hours before you can go
home. It’s normal to have a little bit of spotting or bleeding
afterward.
Treat Yourself Well
Be good to yourself during your
pregnancy. Light some candles and soak in the tub. Go to your
hairdresser for some pampering. Download some of your favorite music to
your iPod or MP3 player. Rent a tear-jerker movie, and cry your eyes
out. Buy yourself flowers. Get a pedicure even if you can’t see your
feet anymore.
At about 36 weeks or when you go into
labor, the stitch is removed, and baby can be born normally. The suture
is removed in labor and delivery without anesthesia. It takes about 5
minutes. Labor does not necessarily happen immediately after it’s
removed; it can occur in a few days to a few weeks.
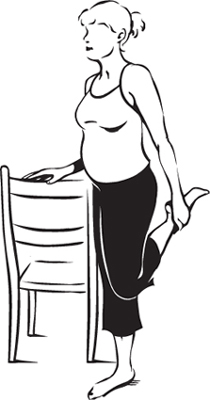
Exercise for Week 24
Stand with your right side against the
back of the sofa or a sturdy chair. Hold onto the back with your right
hand. Bend your knee, and bring your left foot up behind your bottom.
Grasp your foot with your left hand. Keeping your right knee slightly
bent, hold for 10 seconds. Repeat for your right leg. Strengthens quadriceps.