1. How Big Is Your Baby?
By this week, your baby weighs about 5¾
pounds (2.6kg). Its crown-to-rump length is over 13½ inches (34cm), and
total length is 18⅔ inches (47cm).
2. How Big Are You?
From the pubic symphysis, it’s
about 14½ inches (36cm) to the top of the uterus. From your
bellybutton, it’s more than 5½ inches (14cm) to the top of the uterus.
3. How Your Baby Is Growing and Developing
An important part of your baby’s
development is maturing of its lungs and respiratory system. The
respiratory system is the last system to mature. Knowing how mature a
baby’s lungs are helps in deciding about early delivery, if it must be
considered. Tests can predict whether baby will be able to breathe
without assistance.
Respiratory-distress syndrome (RDS) or hyaline membrane disease
occurs when lungs aren’t completely mature, and baby can’t breathe on
its own after birth. The baby may require a machine to breathe for it.
Several fetal-lung-maturity tests can be
done. The test done depends on availability of the test in your area
and the experience of your health care team. Your healthcare provider will determine if a test is necessary and which one to do.
Two methods for evaluating fetal-lung maturity require amniocentesis. They are discussed below.
The L/S ratio is done around 34
weeks of pregnancy. The ratio in amniotic fluid changes between
lecithin and sphingomyelin at this time. Levels of lecithin increase,
while levels of sphingomyelin stay the same. The ratio between the two
levels indicates if a baby’s lungs are mature.
The phosphatidyl glycerol (PG)
test is the second way to evaluate lungs. The test is positive or
negative. If phosphatidyl glycerol is present in amniotic fluid
(positive), the infant will probably not have respiratory distress at
birth.
4. Changes in You
You have only 4 to 5 weeks until your due
date. You may have gained 25 to 30 pounds (11.25 to 13.5kg), and you
still have a month to go. It isn’t unusual for your weight to stay the
same or change very little at your weekly visits after this point.
The maximum amount of amniotic
fluid surrounds the baby now. In the weeks to come, the baby continues
to grow, but some amniotic fluid is reabsorbed by your body. This
reduces the amount of room in which the baby has to move. You may
notice a difference in baby’s movements. For some women, it feels as if
baby isn’t moving as much as it has been.
Restless-Leg Syndrome (RLS)
You may have restless-leg syndrome (RLS)
for the first time during pregnancy; it can rob you of sleep. If you
develop RLS, you will feel a sensation in your legs that makes you feel
as if you must move your lower limbs. Experts suggest RLS may be linked
to anemia and could be caused by an iron or folic-acid deficiency.
Treatment includes increasing your iron intake and taking folic acid. Talk to your doctor before
you do either. Applying a heating pad for 15 to 20 minutes may help.
The good news is RLS often disappears completely after baby’s birth.
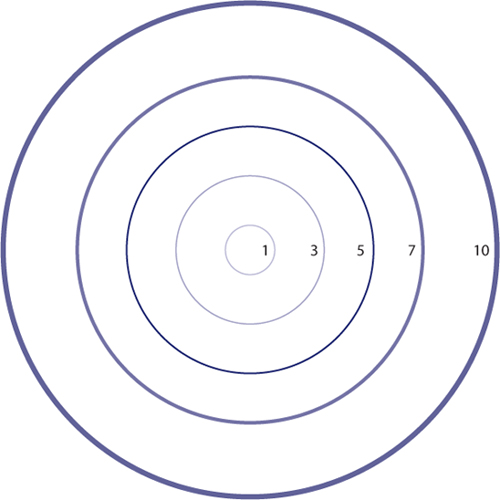
Cervical dilatation in centimeters (shown actual size).
What Is Labor?
It’s important to understand the labor process. You’ll be more informed when labor occurs, and you’ll know what to do. Labor
is defined as the stretching and thinning (dilatation) of your cervix.
This happens when the uterus, which is a muscle, tightens and relaxes
to squeeze out the baby. As the baby is pushed out, the cervix
stretches. Your cervix must open to 10cm (about 4 inches) for your baby
to pass through it. (See the cervical dilation chart on the opposite
page.)
We don’t know what causes labor to begin,
but there are many theories. One is that hormones made by the mother
and baby together trigger labor. It’s believed both release the hormone
oxytocin, which triggers labor. Or it could be the baby produces some
hormone that causes the uterus to contract.
The cervix must also soften and thin out
(become effaced). To put it in more understandable terms, before
pregnancy, your cervix is about as hard as the end of your nose. Close
to delivery, it is about as soft as your ear lobe.
At various times, you may feel tightening, contractions or cramps, but it isn’t actually labor until there is a change in the cervix. As you can see from the discussion below, there are many aspects to labor. You’ll go through them all to deliver your baby.
Three Stages of Labor. There are three distinct stages of labor.
• Stage one—The first stage
of labor begins with uterine contractions of great enough intensity,
duration and frequency to soften and dilate the cervix. The first stage
ends when the cervix is fully dilated (10cm) and open enough to allow
baby’s head to come through it.
• Stage two—The second stage of labor begins when the cervix is completely dilated at 10cm. This stage ends with the delivery of baby.
• Stage three—The
third stage of labor begins after baby’s birth. It ends with delivery
of the placenta and the membranes that have surrounded the fetus.
Some doctors have described a fourth
stage of labor, referring to a time after delivery of the placenta
during which the uterus contracts. Contraction of the uterus is
important in controlling bleeding after delivery.
How Long Will Labor Last? The length of the first and second stages of labor can last 14 to 15 hours or more in a first pregnancy. The average length of active labor is between 6 and 12 hours. When you hear about a long labor,
most of the time is spent in early labor. Contractions may start and
stop or be weaker or farther apart, then get regular and strong.
A woman who has already had one or two
children will probably have a shorter labor, but don’t count on that
either! The average time for labor usually decreases by a few hours for
a second or third delivery.
Everyone’s heard of women who barely made
it to the hospital or had a 1-hour labor. For every one of those women,
there are others who have labored 18, 20, 24 hours or longer. It’s
impossible to predict the amount of time that will be required for
labor. You may ask your healthcare provider, but his or her answer is
only a guess.
Every labor is different, in great part because of the level of pain you experience. Be aware that contractions can hurt.